
The following are the main Cardiovascular conditions that can be treated by Doctor Villa. For detail information, click on desire condition:
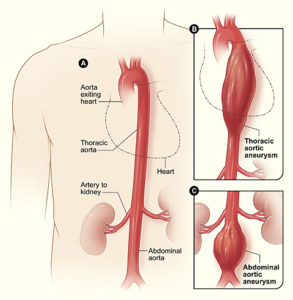
What is Aneurysm?
An aneurysm is a permanent ballooning in the wall of an artery. The pressure of blood passing through can force part of a weakened artery
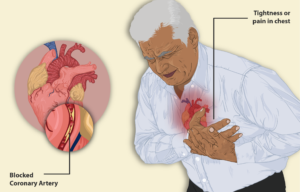
What is Angina?
Angina is chest pain or discomfort that occurs if an area of your heart muscle doesn”t get enough oxygen-rich blood. Angina may feel like pressure
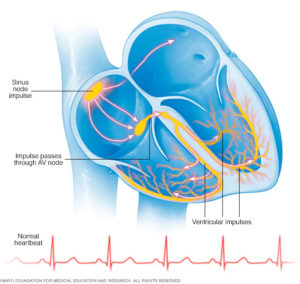
What is Arrhythmia?
Arrhythmias are heart rhythm problems that occur when the electrical impulses in your heart that coordinate your heartbeats don”t work properly, causing your heart to
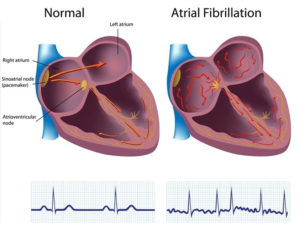
What is Atrial Fibrillation?
Atrial fibrillation is the most common irregular heart rhythm that starts in the atria. Instead of the SA node (sinus node) directing the electrical rhythm,
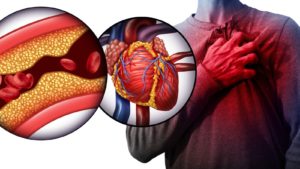
What is Cholesterol?
What is Cholesterol? Cholesterol is a fatty substance, also called a lipid, that”s produced by the liver. It”s also found in foods high in saturated
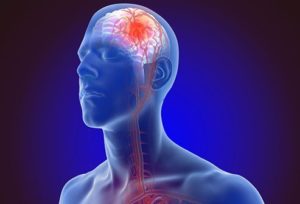
Stroke
A stroke, or cerebrovascular accident (CVA), occurs when blood supply to part of the brain is disrupted, causing brain cells to die. When blood flow
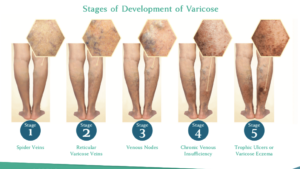
Superficial Venous Reflux
What is superficial venous reflux? Superficial venous reflux is a condition that develops when the valves that usually keep blood flowing out of your legs

Ventricular Fibrillation
Ventricular fibrillation is a life-threatening abnormality in the electrical rhythm of the nerves of the ventricular portion of the heart. In this case, the rhythm
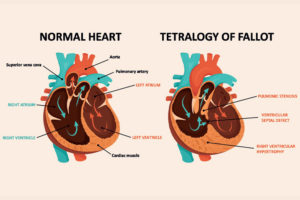
What are Congenital Heart Defects?
What is a Congenital Heart Defect? A congenital heart defect is an abnormality in any part of the heart that is present at birth. Heart
What is Coronary Heart Disease?
What Is Coronary Heart Disease? Coronary heart disease (CHD), also called coronary artery disease, is a condition in which plaque builds up inside the coronary
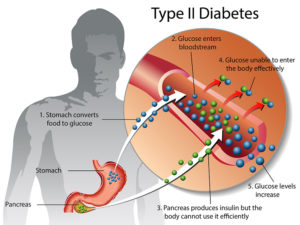
What is Diabetes Mellitus Type 2?
Definition Diabetes mellitus type 2 is a chronic condition that affects the way your body metabolizes sugar (glucose), your body”s main source of fuel. With
What is Endocarditis?
What is Endocarditis? Endocarditis is an infection of the inner lining of your heart (endocardium). Endocarditis typically occurs when bacteria or other germs from another

What is Heart Attack?
What is a Heart Attack? A heart attack usually occurs when a blood clot blocks the flow of blood through a coronary artery. A coronary
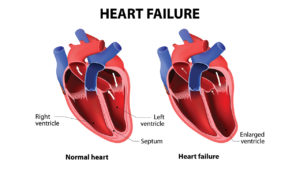
What is Heart Failure?
What Is Heart Failure? Heart failure is a condition in which the heart can”t pump enough blood to meet the body”s needs. In some cases,
What is High Blood Pressure/ Hypertension?
Blood is carried from the heart to all the body”s tissues and organs in vessels called arteries. High blood pressure (HBP), or hypertension, means high
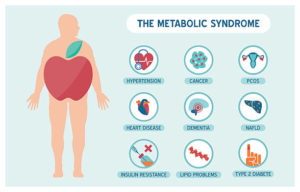
What is Metabolic Syndrome?
What is Metabolic Syndrome? Metabolic syndrome is a collection of heart disease risk factors that increase your chance of developing coronary heart disease related to
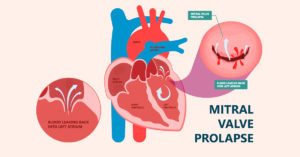
What is Mitral Valve Prolapse?
The mitral valve controls the flow of blood into the left ventricle. Normally, when the left ventricle contracts, the mitral valve closes and the blood

What is Obesity?
Although used interchangeably, “overweight” and “obese” do not mean the same thing. Obesity is a medical term meaning the storage of excess fat (adipose tissue)
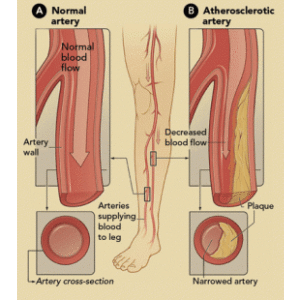
What is Peripheral Artery Disease (PAD)?
Peripheral heart disease is also known as peripheral vascular disease, peripheral heart disease, or PAD. It affects the blood vessels outside the heart, causing it
What is Pulmonary Hypertension?
Pulmonary hypertension is high blood pressure of the arteries in the lungs – which can lead to heart failure. Patients with pulmonary hypertension experience shortness

What is Stress?
Stress has become well known as a major factor to one”s heart health. Stress can directly cause heart conditions, such as hypertension, through repeated elevations
